Slide Show - Understanding Myelodysplastic Syndromes
This slide show provides an overview of myelodysplastic syndromes (MDS), and describes the causes, risk factors, symptoms, and different types of MDS. It also explains the role of bone marrow to produce blood cells (red blood cells, white blood cells, and platelets) and what happens to normal bone marrow in MDS.
Click here to take our SURVEY
Your feedback is important to us! We will use your feedback to develop future areas of content about MDS which will help other patients, caregivers and families.
Animation - Understanding Myelodysplastic Syndromes
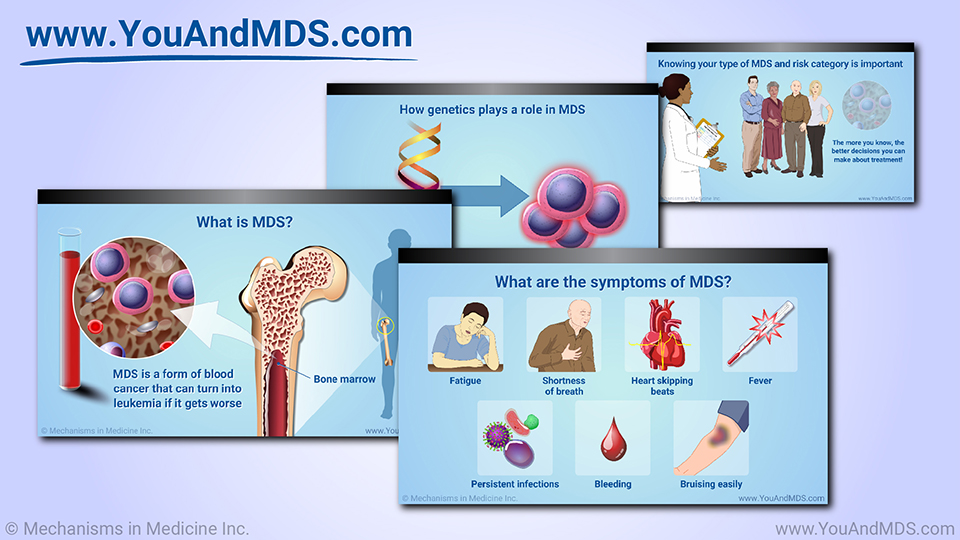
Slide Show - Understanding Myelodysplastic Syndromes

1.
What is MDS?

2.
What causes MDS?

3.
What are the symptoms of MDS?

4.
What are the risk factors for MDS?

5.
Can MDS be prevented?

6.
Is MDS hereditary? Does genetics play a role?

7.
What are the types of MDS?

8.
How is MDS classified?

9.
How serious a cancer is MDS? What is the prognosis for MDS?

10.
George's story: How did you find out you had MDS?

11.
George's story: What has been the biggest challenge for you with your MDS?

12.
George's story: What has been the biggest surprise for you with your MDS?

13.
George's story: What advice do you have for other patients on their journey with MDS?

14.
David's story: What advice do you have for other patients on their journey with MDS?